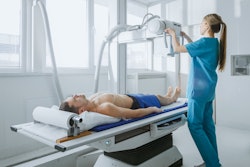
Radiologic technologist aides may take on an expanded role in health systems facing technologist shortages, according to research published March 25 in Current Problems in Diagnostic Radiology.
Radiologic technologist aides who were trained in sterile technique and ultrasound setup supported interventional radiology (IR) services in a study led by Julie Mucciarone from Massachusetts General Hospital in Boston and colleagues.
“Training radiologic technologist aides to assist with sterile preparation and ultrasound-guided workflows helped preserve procedural access to care,” the Mucciarone team wrote.
Health systems and radiology departments continue to face staffing challenges. A 2025 survey conducted by the American Society of Radiologic Technologists (ASRT) showed that vacancy rates for all medical imaging disciplines are above the rates reported in 2020. From 2023 to 2025, vacancies increased for CT, MRI, and bone densitometry.
Mucciarone and colleagues studied the efficacy of a quality improvement initiative conducted in Massachusetts General Hospital’s IR department in 2024 and 2025. This followed the closure of a fluoroscopic procedure room due to radiologic technologist shortages.
The initiative included training radiologic technologist aides in sterile technique and ultrasound setup to assist with bedside and non-fluoroscopic procedures performed under Advanced Practice Provider (APP) or physician supervision.
Final analysis included 1,048 IR procedures, with radiologic technologist aides participating in 205 cases (19.6%). This included 115 APP-supervised cases and 90 physician-supervised cases.
Aides had the most involvement in ultrasound-guided procedures (n = 147), followed by non–image-guided cases (n = 37) and fluoroscopic cases (n = 21). The aides always worked with a technologist for the fluoroscopic cases.
Among APP-led cases, aides most commonly supported ultrasound-guided drainage procedures (n = 69) and non–image-guided tunneled catheter or port removals (n = 34). Among physician-led cases, aides most frequently supported ultrasound-guided venous ablation/sclerotherapy (n = 53) and drainage procedures (n = 20).
The researchers reported no complications that could be attributed to aide involvement.
Using RT aides could be a sustainable strategy to address IR workforce shortages, the study authors highlighted.
“While such models may improve procedural productivity when assessed by case volume alone, they also redistribute clinical workload in ways that are not fully captured by traditional productivity metrics,” they wrote.
However, they also noted that APPs and physicians assume greater responsibility for workflow coordination, sterile field management, and procedural support when aides perform this work.
“These considerations underscore the importance of evaluating provider workload and sustainability, in addition to throughput, when implementing alternative staffing models,” the authors added.
The team suggested that future directions could include expanding APP training for broader independent ultrasound practice, exploring formal certification pathways for APPs to deliver fluoroscopy, and evaluating whether radiologic technologist aides can perform more procedure types.
Read the full study here.